In part 1 of this series, we learned about four types of stress we can face during times of crisis. If left unchecked, these stressors can eat away at our physical, mental, and emotional reserves and eventually put us at risk for stress-related illnesses like PTSD, substance abuse, clinical anxiety, and clinical depression.
The world is still reeling from one crisis: COVID-19. McKinsey & Company has reported on the pandemic’s economic impact across multiple industries, including restaurants, banks, education centers, auto makers, insurers, and healthcare systems.
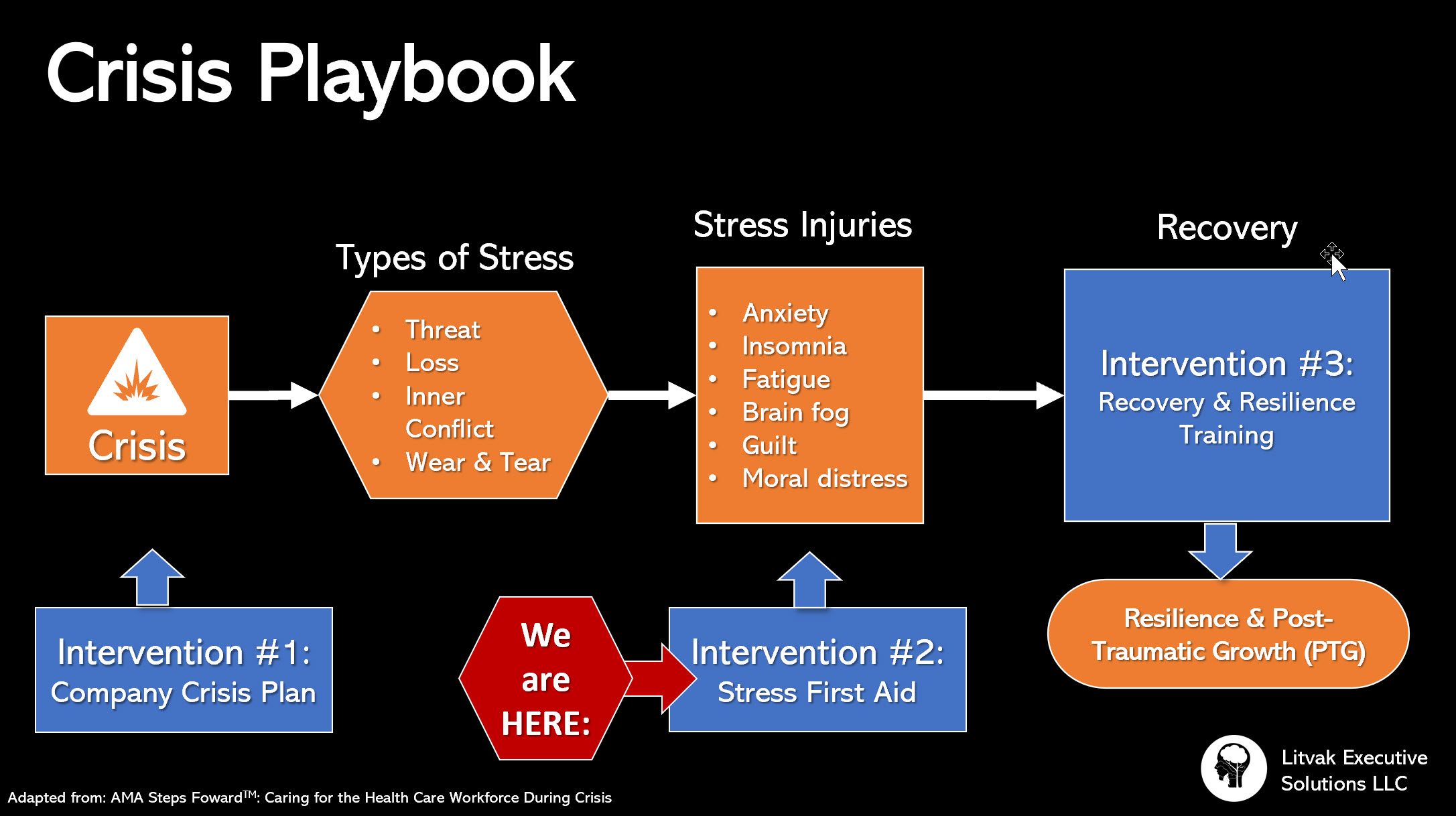
Illustration by Pamela Coburn-Litvak
Since I specialize in coaching healthcare leaders, I’m paying close attention to crisis guidance provided by the American Medical Association. In this article, we are ready to move on to intervention step #2: applying Stress First Aid (SFA).
How do we know what SFA to apply during a crisis? Research teams headed by Dartmouth psychiatrist Patricia Watson have worked out the answer: figure out what has worked for those in high-stress and high-risk jobs like the military, fire and rescue, and law enforcement, and then apply those principles to other workers in crisis. In 2020, Dr. Watson worked with her colleagues William Nash of the United States Marine Corps and Richard Gist from the Kansas City Fire Department to publish a new version of the SFA model for healthcare workers dealing with the COVID-19 crisis (available here).
The Stress Continuum Model
Watson, Gist, and Nash’s SFA model is based on a key fact about stress: we experience stress on a continuum.

Illustration by Pamela Coburn-Litvak
It doesn’t matter what kind of job you have – you’ve probably already noticed this. In the green or “ready” zone, you and I have just the right amount of stress to keep us engaged and challenged, but not so much that we feel overwhelmed and burned out. We feel calm, confident, and in control. This level of stress doesn’t pose any risk – in fact, it probably means you and I are humming along happily in our personal and professional lives.
But then a more severe stressor hits, which move us into the yellow or “reacting” zone. This level of stress is enough to knock us off our game just a bit. You and I may feel tense and frustrated, but usually we can resolve the stress in a short time and move back into the green zone.
Even more severe stress can push us into the orange or “injured” zone. These are crisis conditions that involve one or more of the types of stress we described in part 1. And it’s not so easy to bounce back from this kind of stress. You and I may feel upset and angry, panicked, or depressed. We will almost certainly feel like things are beginning to spiral out of control.
Our ability to move back into the green zone will depend on several things: the severity of the stress, your or my past history with stress and trauma, our biological and psychological risk factors to stress-related mental illness like anxiety and depression, and our respective levels of resilience.
If we can’t resolve our stress, you and I may ultimately end up in the red “ill” zone where we are at high risk for developing stress-related illnesses like PTSD, substance abuse, and clinical anxiety and/or depression.
The whole point of stress first aid is to help us move navigate the orange/red zones of stress successfully and bring us safely back into the green/yellow zones.
The Seven Cs of Stress First Aid
Research shows that we recover best from crisis when our stress first aid kit includes five essential elements:
- Cover. Providing safety is of paramount concern during crisis. This includes not only physical safety, but psychological safety as well – making sure that workers are able to express their concerns and fears without judgement or retribution. After workers’ basic needs are met, company leaders should make sure that they feel mentally and emotionally safe as well.
- Calm. Some anxiety during crisis is normal – healthy, even. Anxiety is nature’s way of keeping us on our toes, helping us stay alert and focused on the crisis at hand. But problems will arise if we stay in a state of anxiety for too long. Not only does this produce bad physiological effects like high blood pressure, ulcers, tension headaches, etc., but it also creates mental and emotional strain in the forms of interrupted sleep, poor focus and decision-making, flared tempers and nail-biting worry.
- Connectedness. Research shows that social connections are powerfully protective against stress and are linked to emotional well-being and recovery after trauma.
- Competence. Workers who believe they have the skills and capacity to endure and overcome threat generally come out of crisis conditions better than those who don’t.
- Confidence. We could also call this hope or optimism. Workers who believe that things will work out, or that some good can come from bad situations, generally come out of crisis conditions better than those who don’t.
Depending on workers’ needs, company leaders may focus on any one or all five tools in the SFA kit. It’s quite possible that different workers will have different needs, and their needs may also change over the course of the crisis. So, company leaders must be able to monitor and adjust their first aid strategy with changing circumstances. To do this, we add two more elements to the toolkit:
- Check. Company leaders must assess, observe, and listen for signs of stress reactions in themselves and others during times of crisis.
- Coordinate. This means getting the information and support needed at every stage of a crisis. A solid crisis management plan is a good start here, but since no one can anticipate the unique challenges of every crisis (hello, COVID-19), leaders must be ready to gather additional information and resources as needed.
Together, these create the seven Cs of Stress First Aid:

Illustration by Pamela Coburn-Litvak
Click on the tabs below to learn how to implement each step of the Stress First Aid (SFA) model:
Conclusion
For more information on the Stress First Aid model, please see the original document developed for healthcare workers here, which also includes a SFA group exercise and suggested questions to ask for each step in the model.

