State of Well-being (and Burnout) in Healthcare
If you are a healthcare professional or administrator, chances are you know about the Well-being Index (WBI). Developed by clinicians at the Mayo Clinic, this 9-question survey helps healthcare institutions assess 6 dimensions of emotional distress – and its converse, well-being – in their workforce.
The Well-being Index has been a crucial tool, especially over the last couple of years as healthcare professionals have navigated the greatest public health crisis in 100 years. The WBI is free for individual use and is also licensed by healthcare organizations around the world. You can access the tool and download case studies and reports at the WBI website.
WBI staff also publish the latest well-being data and trends among healthcare workers on an annual basis. I just finished reading the latest report, The State of Well-being 2021-2022. As always, they did an excellent job of elucidating key findings about well-being/burnout over the past year.
And just what exactly did they find? That’s what I will spend the rest of the article reviewing.
The short version is this: a majority of healthcare professionals (over 60%) are experiencing significant emotional distress and burnout. A little more than half (51%) are seeking professional help for stress-related issues. Considering the year we just had, these findings are not particularly surprising, but still concerning.
Now for the longer version.
The Burden of Burnout in Healthcare
For context, let’s first talk about the massive burden of burnout in healthcare. Research has described in excruciating detail the personal and professional consequences of burnout:
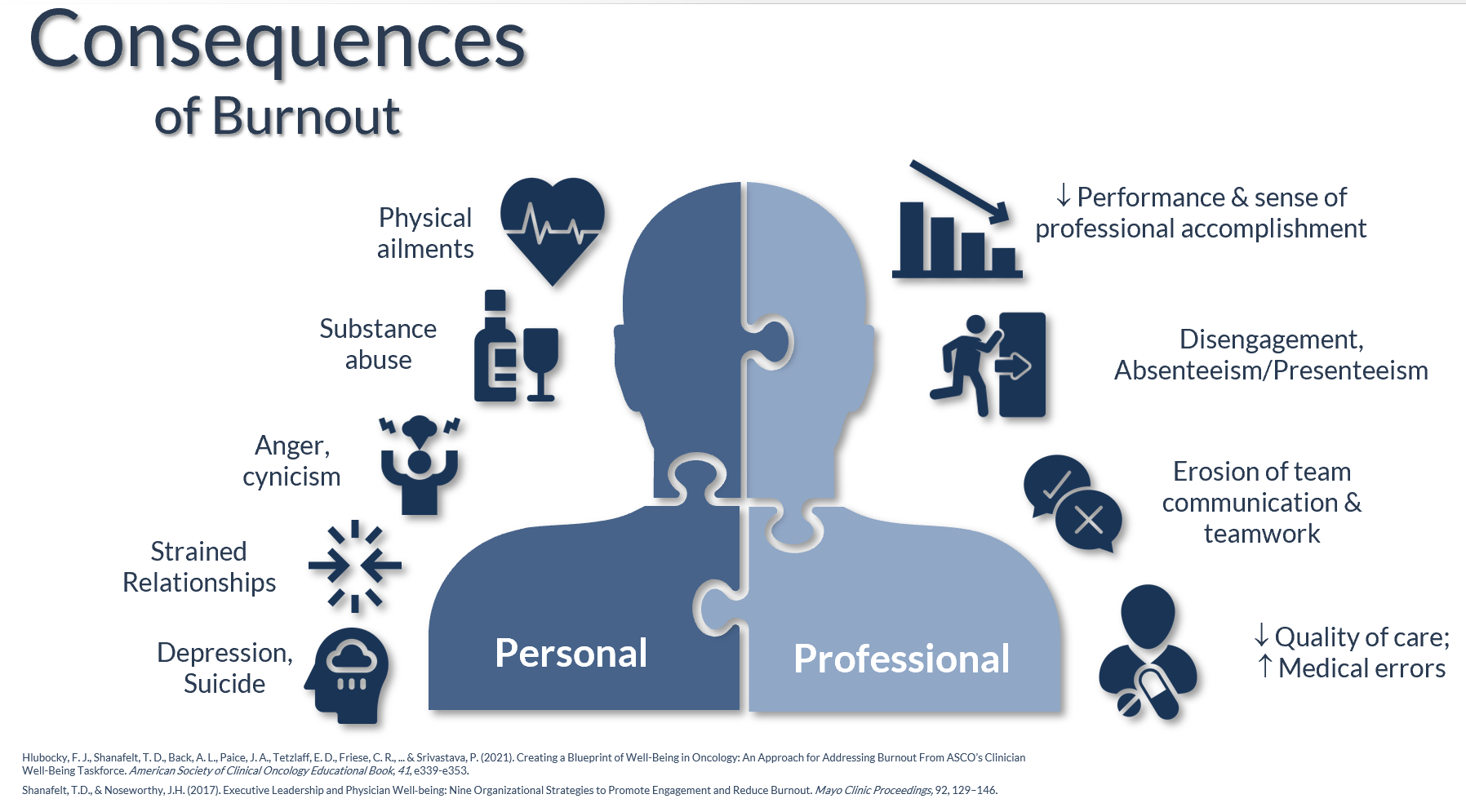
Organizations also bear the consequences of burnout:
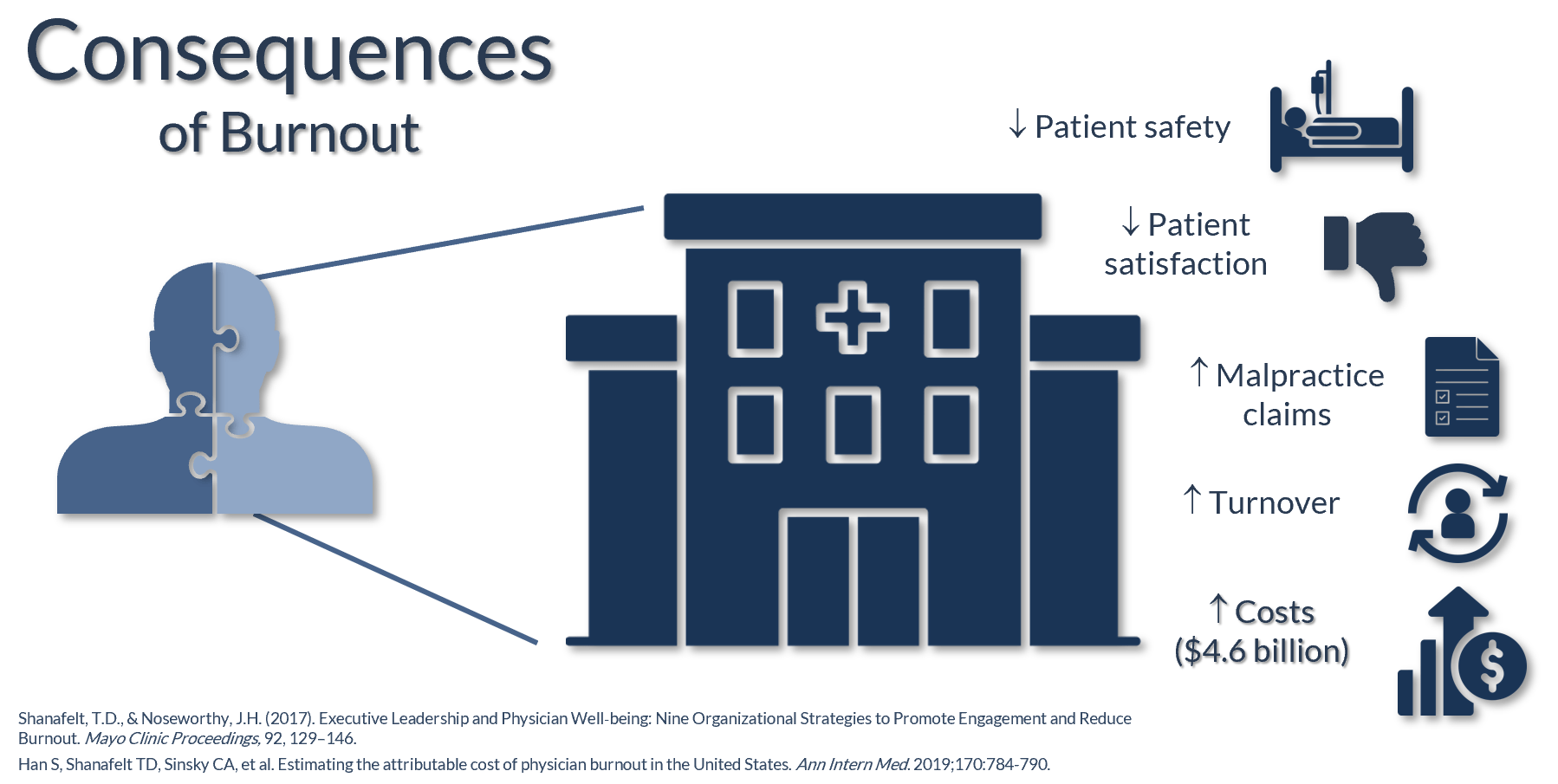
Ultimately, burnout drives up financial costs – an estimated $4.6 billion in physician turnover and reduced clinical hours. This is a moderate estimate if you count in lawsuits and liability costs – researchers think the true cost could be north of $6 billion. The annual cost is roughly $7,600 per employed physician, resulting in lost revenue and also diminished patient satisfaction.
But burnout is costly to everyone involved. It has a nasty, negative effect on every aspect of the Quadruple Aim. Importantly, it puts patients at risk.
This is why WBI staff at Mayo and other organizations invest so much time and resources into monitoring rates of emotional distress and burnout in healthcare.
The timing could not be better to review this data, because healthcare systems are feeling distress and burnout like never before. Covid-19 has turned up the heat on burnout and organizations are in need of solutions.
Healthcare Leaders, do you need resources for burnout?
Click the button to download our FREE burnout now.
Two years into a global heath crisis, how are healthcare professionals doing?
Results of the Mayo Clinic’s State of Well-being 2021-2022
Mayo’s latest report, State of Well-being 2021-2022, is based on 165,000+ assessments. About 70% of survey respondents were female, 26% were male, and 4% did not answer or identified as gender diverse.
The survey results represent multiple types of hospitals and healthcare systems. It reports the cumulative state of well-being in healthcare professionals, but also breaks the data down into seven occupational groups: advanced practice providers, pharmacy professionals, physicians, nurses, residents/fellows, medical students, and general healthcare employees. (For brevity, please note that I’ve omitted findings for students, residents and fellows in this article. This is because those in training have specialized challenges and the solutions may be slightly different.)
A majority of healthcare professionals are now suffering with emotional distress and burnout.
To bottom-line the whole thing: the level of emotional distress measured in healthcare professionals in 2021 exceeded that of 2019 and 2020. Which is probably not a shock to anyone.
Emotional distress is strongly tied to the psychological state of burnout. Again, not a shocker. And research tells us that burnout can manifest in three ways in the workplace: 1) emotional exhaustion, 2) reduced personal accomplishment, and 3) depersonalization, which means flagging enthusiasm and a rising sense of cynicism about one’s work.
The latest WBI report indicates that healthcare professionals are feeling the first two, but not necessarily the third, component of burnout:
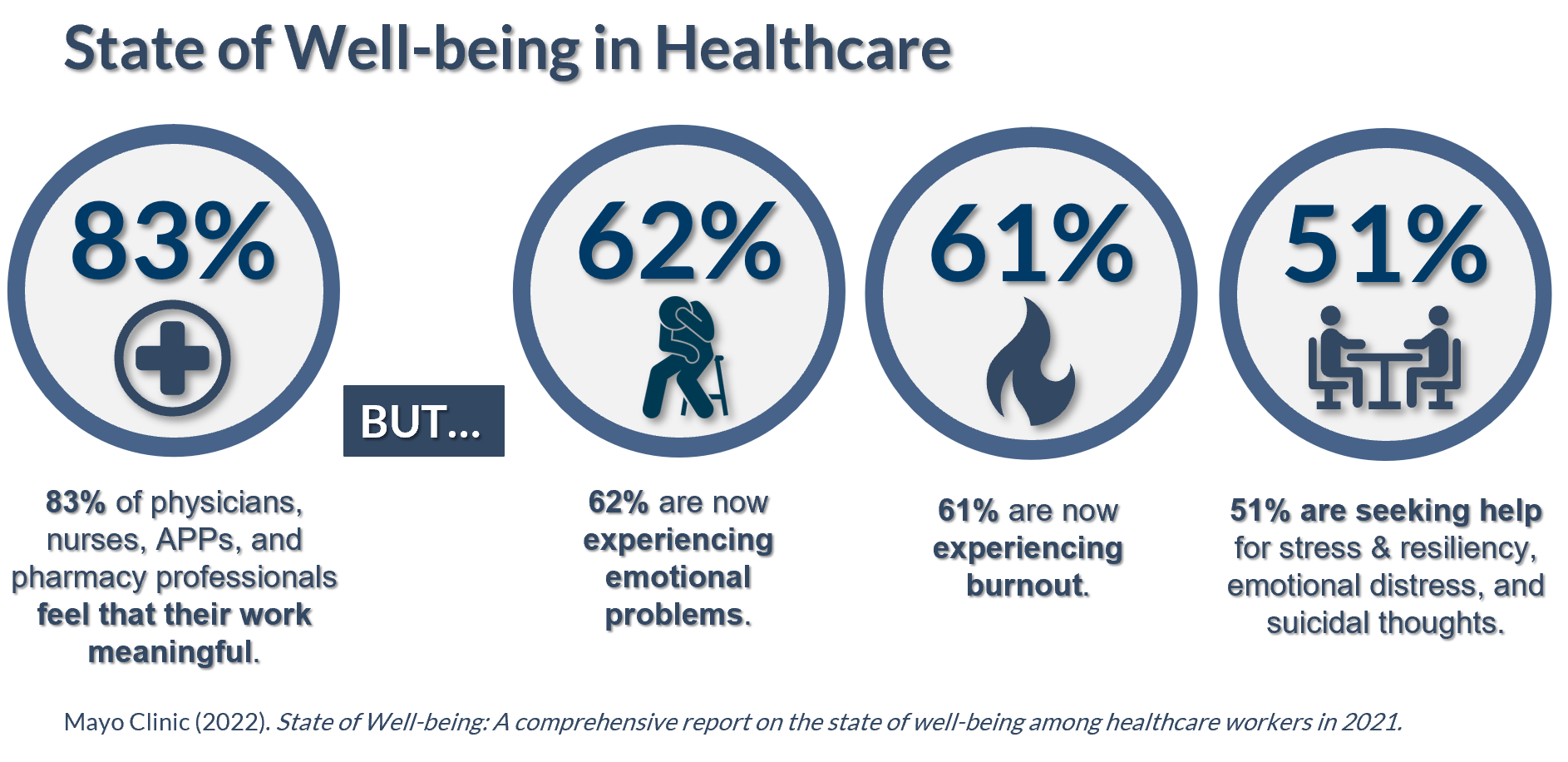
On average, over 8 out of every 10 (83%) healthcare professionals believe that their work is meaningful. This isn’t to say that they don’t get frustrated and overwhelmed by their work at times, and in that sense they experience the depersonalization aspect of burnout as well. But generally speaking, healthcare professionals enjoy a profound sense of personal meaning in their work.
Then the data inserts a big BUT. Despite believing in the value of their work, 6 of out every 10 are also experiencing emotional problems (62%) and are struggling with burnout (61%). Five out of every 10 (51%) are seeking professional help in areas like stress management, resilience training, emotional distress, and even coping with suicidal thoughts. That’s nearly twice the 27% who want professional help for work-life balance and over four times the 12% who are seeking help for career development.
How do these numbers compare across specific occupations? For those interested, here are the numbers:
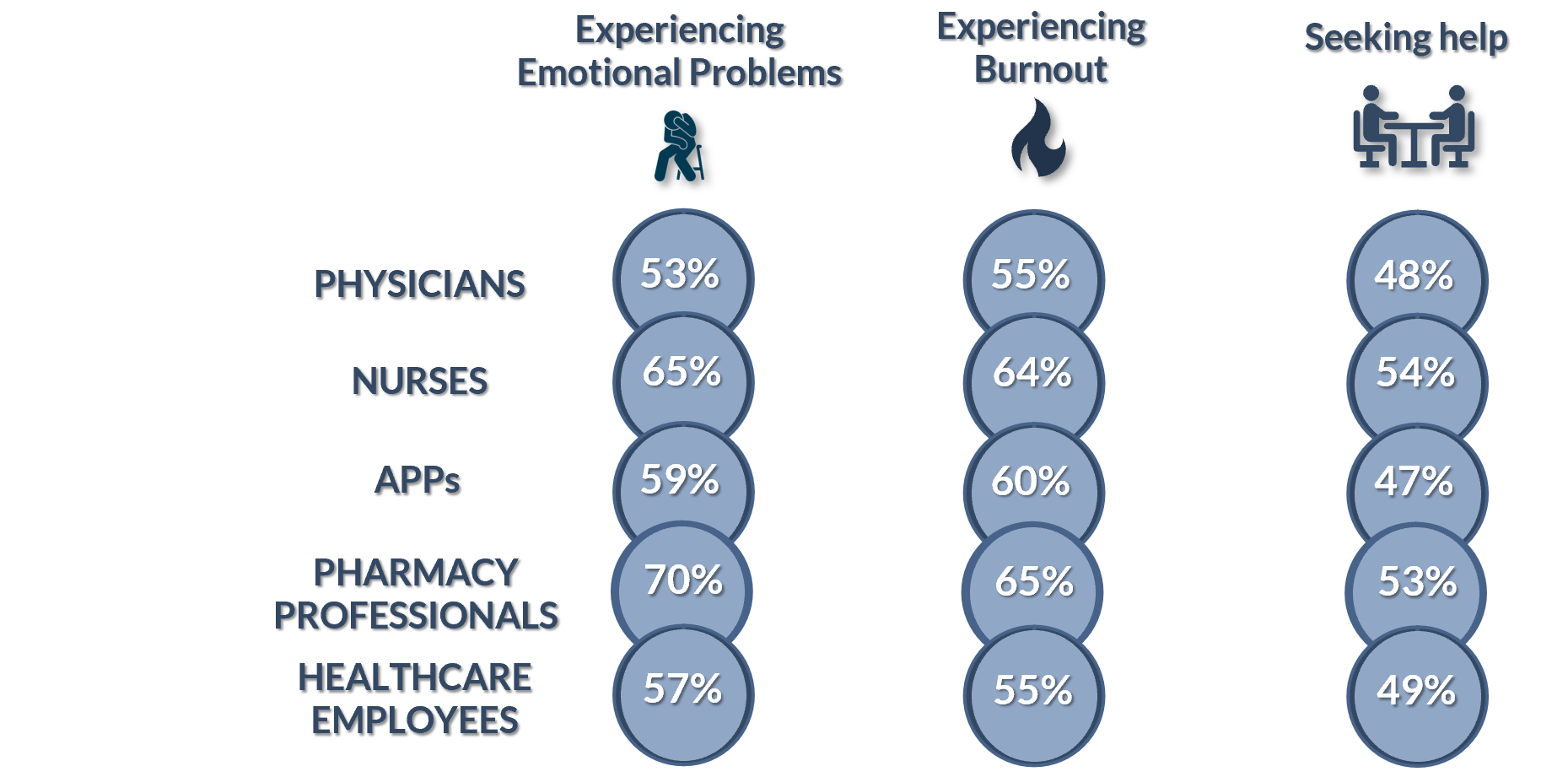
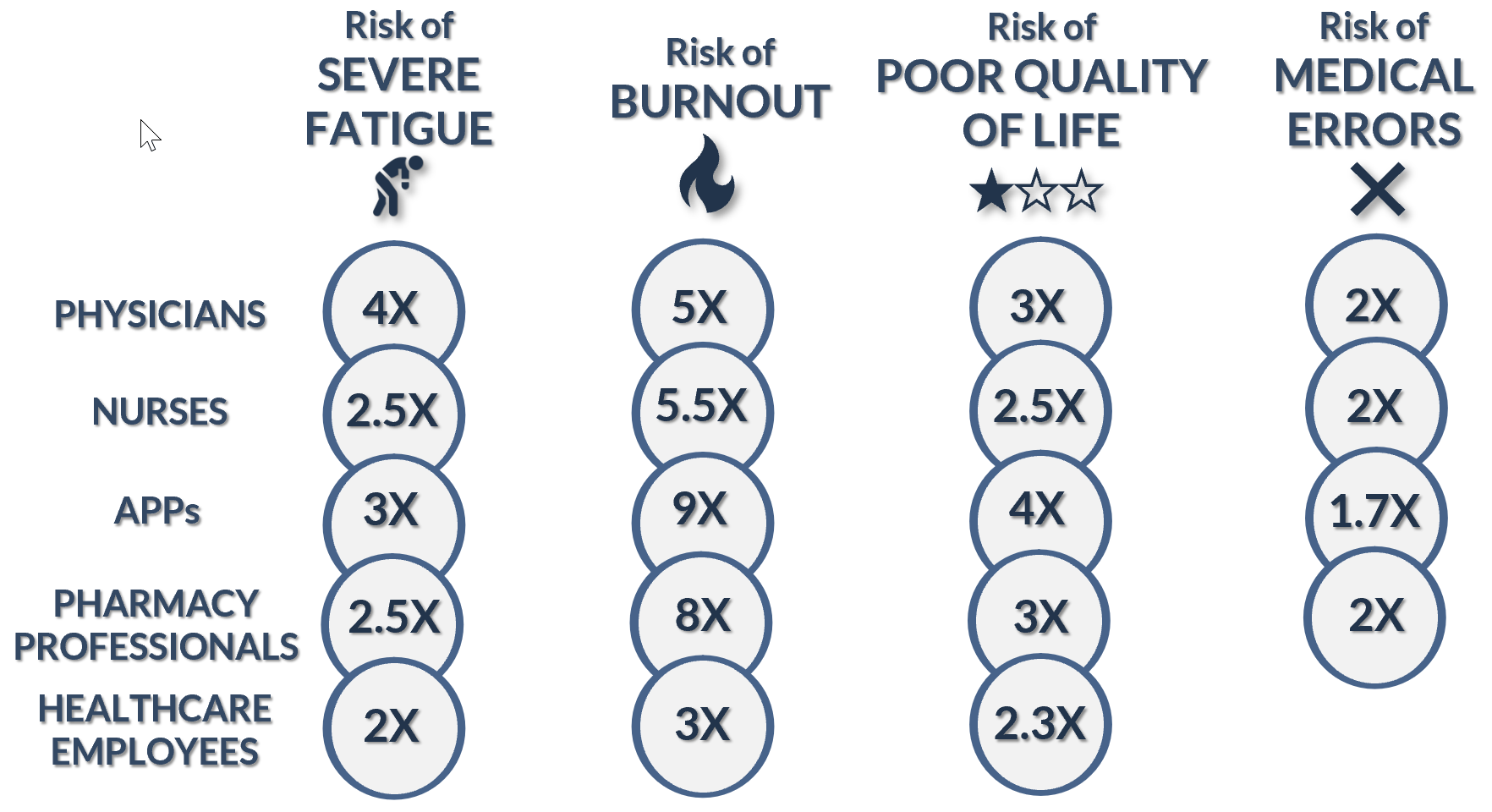
Highly distressed healthcare professionals are at higher risk for severe fatigue, burnout, poor quality of life, and making medical errors.
Survey respondents were deemed to be highly distressed if their WBI score fell beneath a research-validated threshold. And when highly distressed individuals are analyzed separately, they exhibit higher risk for several personal and professional factors.

The 2021 study results reported that, on average, highly distressed healthcare professionals have:
- 3X the risk of severe fatigue;
- 7X the risk of burnout;
- 3X the risk of a poor quality of life; and
- 2X the risk of committing medical errors.
Here are the numbers across healthcare occupations:
Burnout in Healthcare and the Great Resignation
We should ask: are the findings of Mayo’s State of Well-being 2021-22 report corroborated by other studies?
In a word: YES.
In late 2021, market research firm Morning Consult reported that nearly 1 in every 5 healthcare workers had quit during the pandemic. Coming smack in the middle of the Great Resignation that ravaged multiple industries, this report indicated that healthcare was ravaged as well.
Morning Consult also conducted a survey to determine why healthcare workers quit. It’s worth noting that burnout placed fourth on their list of reasons, just behind career-related reasons like better opportunities, compensation, or benefits:
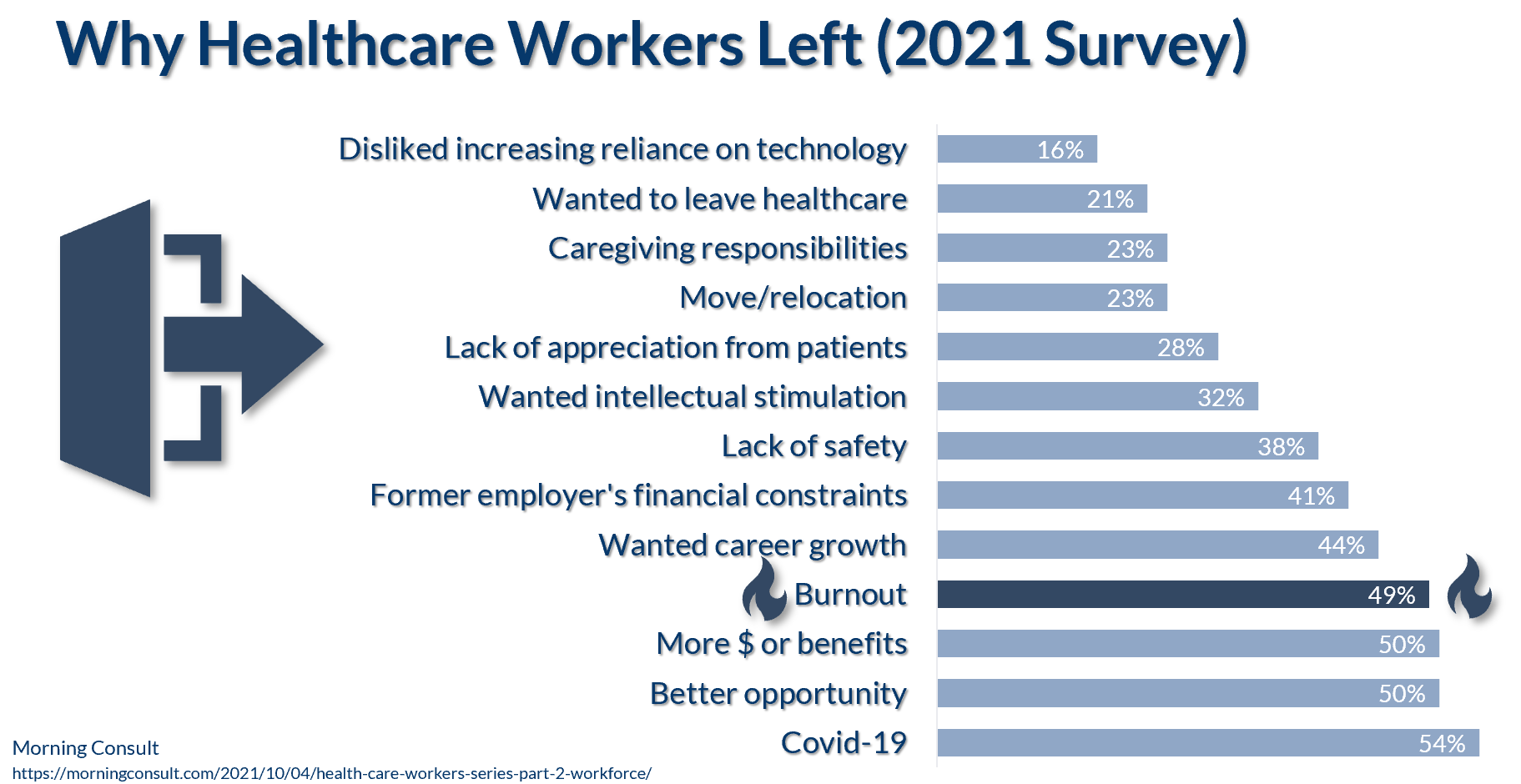
Okay, so industry data from multiple sources is telling the same story. That’s the good news.
The bad news is that the story is grim. Morning Consult quoted one physician as saying, “I have never before in my life seen more physicians feel like they’re almost on a sinking ship…We’re universally feeling the burnout and feeling the pain right now.”
Given its impact, understanding the causes of burnout and implementing interventions is now a strategic imperative for healthcare organizations, leaders, and healthcare professionals themselves.
And here’s some more good news: there are several organizations working on solutions to burnout.
I’m co-leading one of those organizations.
Introducing the Rebound Program!
I am excited to announce the Rebound Program, a collaboration with leadership expert Kate Collins of Brightpoint Coaching & Consulting.
Kate and I are basing our consulting approach and leadership content on decades of research in stress & burnout, employee engagement, and best practices in organizational/leadership development.
We firmly believe – as do most experts – that addressing burnout is a shared responsibility between organizations and individuals. It’s best accomplished with a combination of individual and organizational interventions, although certainly organizations are more responsible for addressing workplace stressors at their source and creating a culture of well-being.
Some strategies have already been described in the research by industry experts like Tait Shanafelt and Bryan Sexton. Here are some examples:
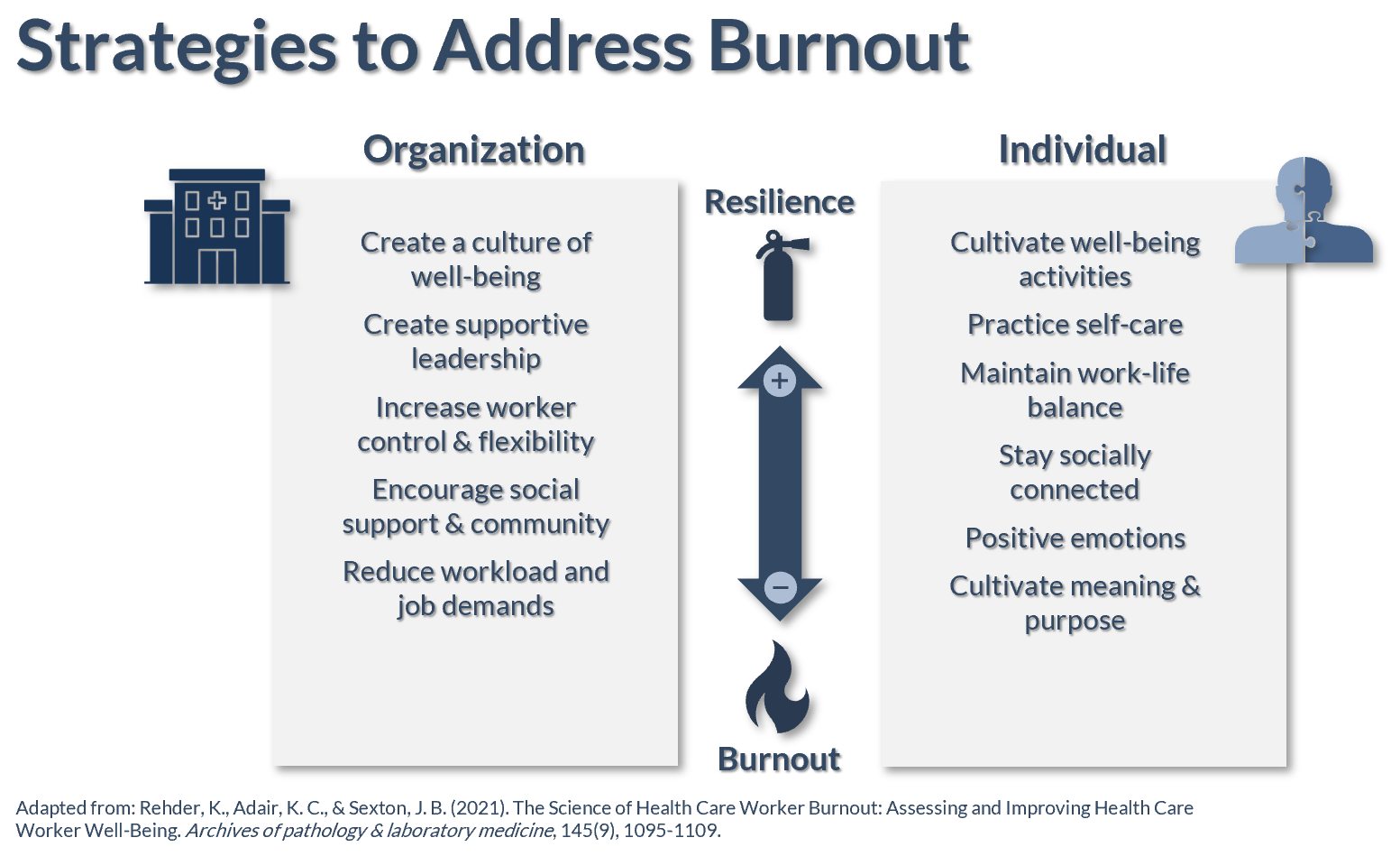
We have developed several solutions from this research, and we invite you to visit https://reboundplan.com to learn more about each:
- Consulting
- Leadership development
- Coaching
- Speaker Series
We also offer several FREE resources, including an organizational toolkit for burnout.
If your organization is suffering from distress and burnout, please contact us. We would love to talk to you!
We help healthcare organizations prevent burnout and promote well-being.
For a FREE toolkit on burnout, click the button below:

