Dr. Anita Sircar is a California-based infectious disease doctor and clinical instructor at the UCLA School of Medicine. In an op-ed for the L.A. Times, she described watching a patient, a healthy man not yet 50 years old, die of Covid-19.
Written nearly 18 months into the pandemic, her words are heavy with frustration and fatigue. Despite doing everything she could for this man, he died anyway, leaving a wife and two young children behind.
It’s a tragic story that, as of this writing, has played itself out over 5 million times worldwide. In the United States alone, over 750,000 people have died of Covid-19.
Summing up her despair, Dr. Sircar wrote, “For those of us who hadn’t left after the hardest year of our professional lives, even hope was now in short supply.”
Her words remind me of this quote by Rachel Remen:
“The expectation that we can be immersed in suffering and loss daily and not be touched by it is as unrealistic as expecting to be able to walk through water without getting wet…We burn out not because we don’t care but because we don’t grieve. We burn out because we’ve allowed our hearts to become so filled with loss that we have no room left to care.”[1]
Dr. Sircar is one of perhaps tens of thousands of other frontline healthcare workers currently in the throes of compassion fatigue. This is what researchers describe as the cost of caring for others in physical or emotional pain.
Caring for others can drain our own physical and emotional strength. We feel spent and cynical. We have a hard time empathizing or caring about our clients/patients, co-workers, and even our loved ones.
What is Compassion Fatigue?
Traumatologist Charles Figley, director of the Figley Institute at Tulane University, describes compassion fatigue as the convergence of 3 factors: burnout,secondary trauma, and compassion satisfaction [2].
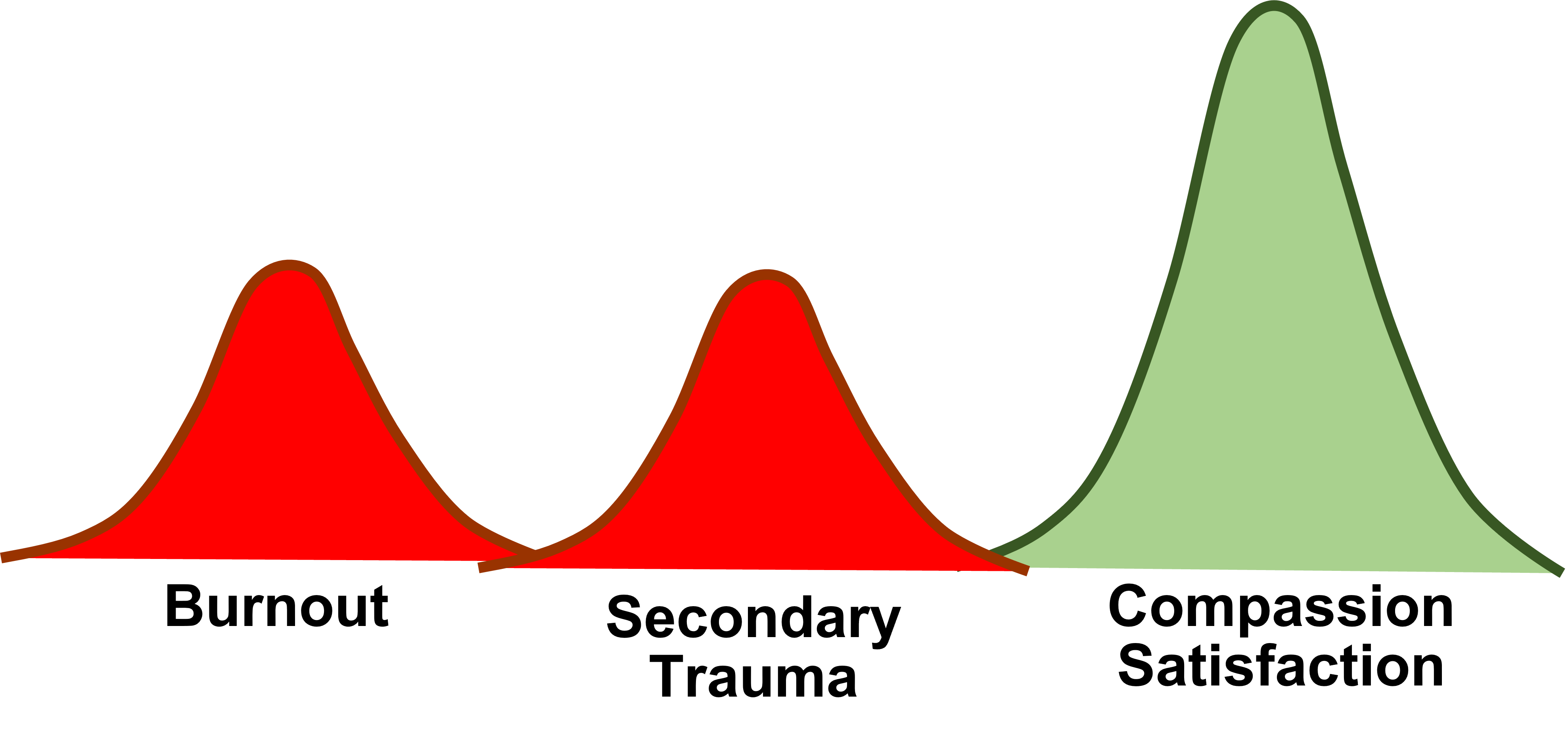
Who Gets Compassion Fatigue?
Compassion fatigue has been on the rise among healthcare workers over the last two years. But we should not lose sight of the fact that this is an occupational hazard for all those who protect and care for others:
- health care workers,
- animal care workers,
- social workers,
- ministers/clergy,
- funeral directors,
- mental health counselors,
- correctional workers,
- military,
- educators, and
- caregivers of relatives (just to name a few).
In some parts of the world, compassion fatigue during Covid-19 was even higher among educators than healthcare workers. Speculating on the reasons why, the researchers wrote, “During those months [of 2020], healthcare workers were considered heroes by most of society. That is, they had the emotional support of a very large number of people who valued and recognized their work. On the contrary, the action of teachers was often severely criticized, as students and their families were going through this situation of uncertainty with heavy overload and stress, frequently attributing the fault to these professionals.”
How Do I Know if I Have Compassion Fatigue?
Since compassion fatigue is a complex, multi-factorial disorder, the symptoms we experience are also complex. They can hit us physically, mentally, and/or emotionally. They can show up in our behaviors and disrupt our relationships.
Here are some symptoms – which ring true for you?
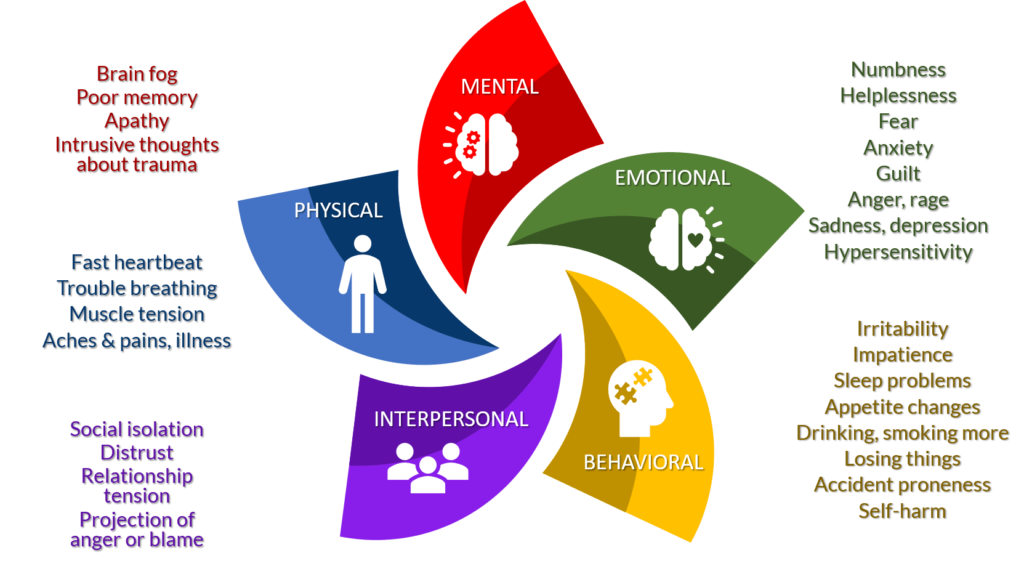
5 Ways to Cope with Compassion Fatigue
1. Understand the Causes.
If you and I can identify the underlying causes of something, we can usually go a long way in resolving it.
As a stress researcher, I wonder about any sources of stress that are feeding into compassion fatigue. Research has identified several, but they can all boil down to two basic categories: who we are and where we work.
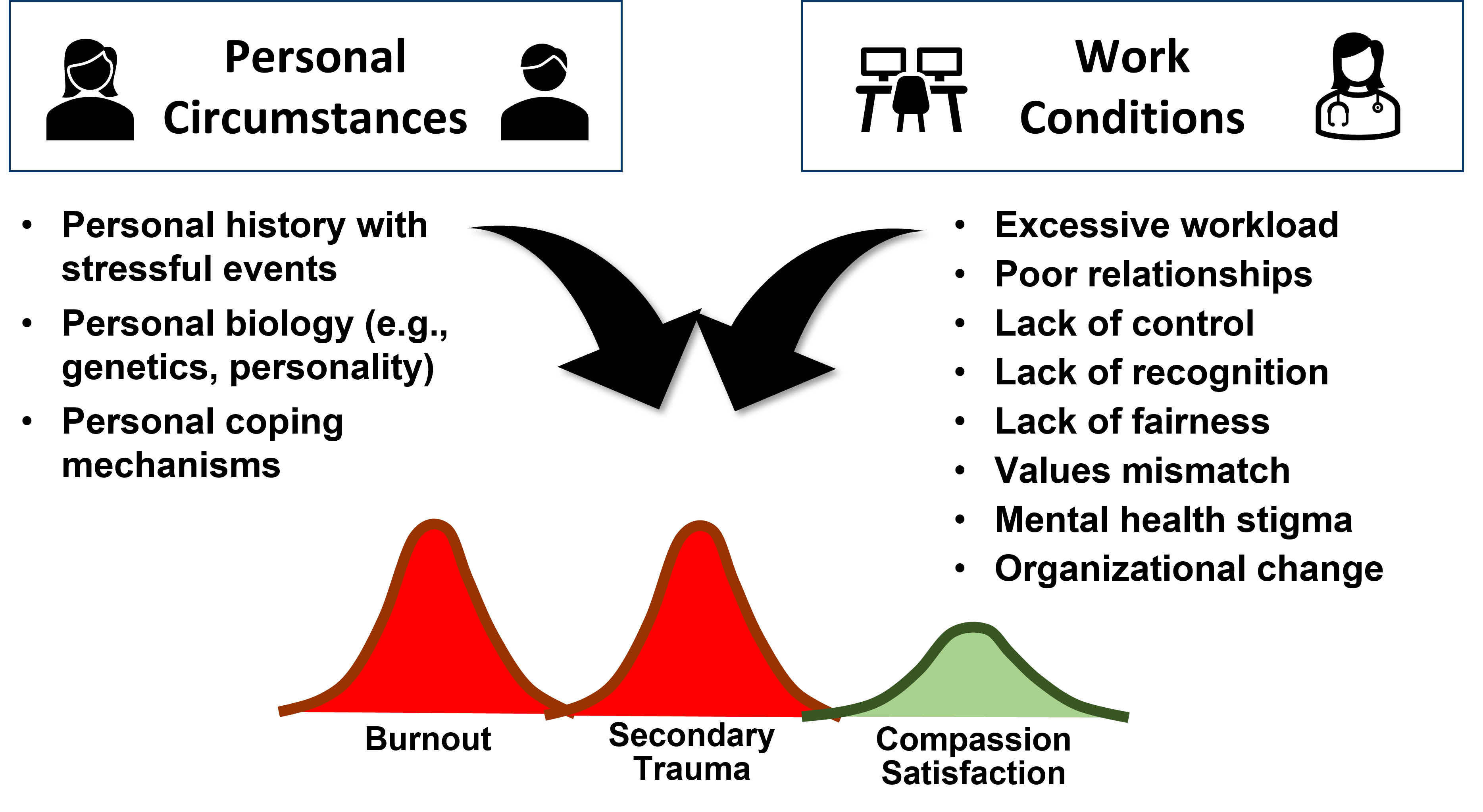
In this first post, let’s focus on our personal circumstances in order to develop personal coping strategies. We’ll get to the work conditions later.
Personal Circumstances (Who We Are)
We are shaped by both biology and life events – in other words, both nature and nurture leave their imprint on us.
- History of Stress: Life events can leave a lifetime impression on us. If we have a history of stress and trauma, especially in early childhood, we are often more sensitive to stress as adults.
- Stress Outside of Work: Few of our colleagues may even be aware that we are struggling with stress at home or in our personal relationships. Yet, we internalize this stress and bring it to work with us. It creates the unstable foundation on which our workplace stress rests.
- Personal Biology: Our genetics and biology can also affect the way we deal with stress. Our sensitivity to stress in the world around us can get amped up or toned down by the way stress hormones and brain chemicals do their thing. Add on to that any personality/psychology quirks that may amplify our stress response, like trait pessimism, e.g., “the glass is half empty” outlook. I’m raising my hand here – I’m a born pessimist and often shuffle around the gloomy side of life rather than the sunny side. But research shows that we “Negative Nancys” (“Negative Neds,” too) generally have a harder time with stress than others do.
- Coping Mechanisms: And add on to that any unhealthy coping mechanisms we’ve picked up along the way, like perfectionism (“Everything has to be perfect, or I’ll tear my hair out”), avoidance (“If I ignore it, it’ll go away”), and/or escapism into drugs, alcohol, comfort foods, etc.
Keep in mind that our personal circumstances are only half the story here. We still need to talk about the work conditions that may be feeding our compassion fatigue. But for the rest of this post, let’s focus on personal coping strategies to combat compassion fatigue.
We’re starting here because this is where you and I personally have the most control. We often can’t do anything about workplace policies and culture. Organizational leaders therefore play a vital role in combatting compassion fatigue, and trust me, I will address that. But as the old saying goes: if we can’t change our circumstances, we can change ourselves. So, that’s where we will begin.
2. Take Care of Yourself.
Caregivers often get so wrapped up in caring for others that they simply forget to care for themselves. But self-care is not a luxury during times of compassion fatigue. It’s a necessity.
Let me repeat that: self-care is not a luxury – it’s a necessity.
This includes all of the stuff you probably knew you should be doing before you started reading this post, like eating right, exercising, getting enough rest, and maintaining good work-life balance.
Often the problem is not that we don’t know what to do, but that we fail to do it.
So, think about why you are not taking care of yourself right now. What’s stopping you? What boundaries do you need to put into your life to protect your mental and physical health?
3. Connect and Care for Others.
I recently wrote about my experience living in New York City right after the 9/11 terrorist attacks.
For a few months afterward, the city changed. Its heart felt more exposed. People flocked to ground zero to hand out sandwiches to the emergency crews. At neighborhood blood drives, people lined up for several blocks to give blood.
There was something else that struck me. Normally, when you use the subways and buses in New York City, the unspoken rule is that you don’t look other passengers in the eye – doing so is considered some sort of challenge or threat.
But for a few months after 9/11, people looked at each other. We searched each other’s faces for signs of pain or fear. And when we saw them, we tried to give each other encouragement: a slight nod, a smile.
This wasn’t just a coincidence. As Elbert Hubbard said, “Suffering makes kinsmen of us all.”
Deep down, we instinctively understand the need to connect when we see – and more importantly, experience – suffering. This is perhaps suffering’s best gift: the ability and the desire to come along someone else and help them through the same thing.
Research unequivocally supports the idea that social connections with loved ones and peers help us build resilience to severe stress. This has held true during Covid-19: in a recent survey of ER nurses, perceived social support protected against compassion fatigue and burnout.
4. Practice Self-Compassion.
There are three key components to self-compassion:
- Practicing self kindness instead of self-judgment. This means extending acceptance, sympathy, and understanding to ourselves when we fail or don’t handle things in a perfect way
- Believing in common humanity rather than isolation. When traumatized, we sometimes isolate ourselves in the belief that “no one can possibly understand what I’m going through.” But suffering – and feeling inadequate in the face of suffering – happens to everyone. It’s part of being human. Therefore, compassion fatigue is not a good reason to shut ourselves off from the rest of the world. On the contrary, in these challenging times, it may be the one thing that all of humanity is experiencing together.
- Being mindful rather than over-identifying. Dr. Kristin Neff puts it this way: “Self-compassion requires a balanced approach to our negative feelings so that they are neither suppressed nor exaggerated.” This comes from doing two things. First, we accept our negative thoughts and explore them in an open, curious, and non-judgmental way (e.g., “This is just where I am right now.”) Second, we remember that we often share our suffering with others. This helps us not over-identify with our own thoughts and feelings and puts them into a larger perspective.
Has self-compassion come in handy during Covid-19? You bet. Healthcare workers have successfully used self-compassion to protect against burnout and compassion fatigue.
5. Find Meaning in Your Work.
The previous four techniques will help reduce the first two factors of compassion fatigue: burnout and secondary trauma. Finding meaning in your work will help boost the third: compassion satisfaction.
What contribution does your work make to the world?
You may have heard the story of President John F. Kennedy touring the NASA space center back in the 1960s. He approached a janitor carrying a broom and asked, “And what do you do here, sir?”
The man threw his shoulders back proudly and said, “Well, Mr. President, I’m helping put a man on the moon.”
What difference does your work make right now and to whom?
Summary and Resources
I’ve focused in this blog post on five powerful strategies that we personally can use to combat compassion fatigue. We’ll get to organizational strategies, too, I promise.
This is such a key issue right now that I’ve created a corporate toolkit as well. You can find it in my online shop, but if you want to try it out first, I’ve created a FREE sample that you can download below. I made sure the free version still provides tons of value, including:
- Summaries of the three factors that create compassion fatigue;
- Recommended assessment tools for each factor;
- 22 specific strategies to use for each factor; and
- Two fillable pdf worksheets from the corporate toolkit: 1) three factors drive compassion fatigue and 2) signs and symptoms of compassion fatigue.
Check it out here:
1. Rachel Naomi Remen: Kitchen Table Wisdom: Stories that Heal, Penguin, New York,1996.
2. Figley, C. R. (Ed.). (2002). Treating compassion fatigue. Routledge.

